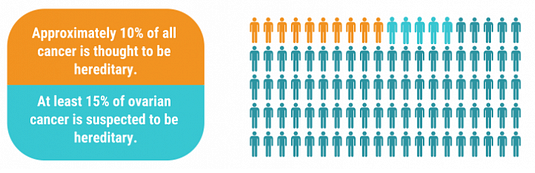
BRCA-Related Breast and/or Ovarian Cancer syndrome is a hereditary cancer syndrome caused by pathogenic variants in the BRCA1 and BRCA2 genes. It results in increased risk for breast, ovarian, prostate, and pancreatic cancers and possibly melanoma. Experts believe genetic risk factors such as BRCA1/2 pathogenic variants are responsible for about 10% of all breast cancers and at least 15% of ovarian cancers. Genetic counseling and testing can help people learn more about their cancer risks and their options for cancer screening and risk-reduction.
Anyone with the following risk factors for BRCA-Related Breast and Ovarian Cancer syndrome should consider seeing a certified genetic counselor to learn more about their risks and whether genetic testing is appropriate:
- History of:
- ovarian cancer
- pancreatic cancer
- male breast cancer
- metastatic or high-risk prostate cancer
- History of breast cancer:
- diagnosed by age 50 or younger
- triple negative breast cancer
- metastatic breast cancer
- multiple separate breast cancers
- History of breast cancer and family history of:
- breast cancer diagnosed by age 50 or younger
- ovarian cancer
- male breast cancer
- pancreatic cancer
- metastatic or high-risk prostate cancer
- two or more relatives with either breast or prostate cancer
- History of prostate cancer and:
- metastatic or high-risk disease
- family history of breast cancer by age 50
- family history of ovarian, pancreatic, or high-risk prostate cancer
- two or more close relatives with either breast or prostate cancer
- Jewish ancestry without additional risk factors
- Family member has a known pathogenic variant in BRCA1 or BRCA2
- BRCA1 or BRCA2 pathogenic variant found in a tumor (known as a somatic variant)
Genetic counseling may still be helpful if someone does not meet the above criteria for genetic counseling themselves, but a close relative does. A genetic counselor can determine whether genetic testing is appropriate and who in the family should be tested first.
Genetic counselors can also help with gaining insurance preauthorization for genetic testing. Insurance coverage for testing varies, but testing is covered for many people with the risk factors listed above.
BRCA status may affect cancer treatment decisions. For example, people with BRCA1 or BRCA2 mutations and certain types of breast, ovarian, prostate, and pancreatic cancers may be offered a type of medication called a PARP inhibitor. They should discuss these treatment options with their oncology team.
In addition to the risk factors listed above, the medical care team should consider other factors when determining a person’s risk, such as family size, number of female relatives, preventive breast and gynecological surgeries, and adoption. A full risk assessment should also consider risk factors for other forms of hereditary cancer.
NCCN Genetic Breast, Ovarian, & Pancreatic 3.2024, Benafif 2015, De Felice 2017, Domchek 2016
This article was updated March 22, 2024.
[/et_pb_text][/et_pb_column][/et_pb_row]
My Gene Counsel ©
BRCA-Related Breast and/or Ovarian Cancer syndrome is a hereditary cancer syndrome caused by pathogenic variants in the BRCA1 and BRCA2 genes. It results in increased risk for breast, ovarian, prostate, and pancreatic cancers and possibly melanoma. Experts believe genetic risk factors such as BRCA1/2 pathogenic variants are responsible for about 10% of all breast cancers and at least 15% of ovarian cancers. Genetic counseling and testing can help people learn more about their cancer risks and their options for cancer screening and risk-reduction.

Anyone with the following risk factors for BRCA-Related Breast and Ovarian Cancer syndrome should consider seeing a certified genetic counselor to learn more about their risks and whether genetic testing is appropriate:
- History of:
- ovarian cancer
- pancreatic cancer
- male breast cancer
- metastatic or high-risk prostate cancer
- History of breast cancer:
- diagnosed by age 50 or younger
- triple negative breast cancer
- metastatic breast cancer
- multiple separate breast cancers
- History of breast cancer and family history of:
- breast cancer diagnosed by age 50 or younger
- ovarian cancer
- male breast cancer
- pancreatic cancer
- metastatic or high-risk prostate cancer
- two or more relatives with either breast or prostate cancer
- History of prostate cancer and:
- metastatic or high-risk disease
- family history of breast cancer by age 50
- family history of ovarian, pancreatic, or high-risk prostate cancer
- two or more close relatives with either breast or prostate cancer
- Jewish ancestry without additional risk factors
- Family member has a known pathogenic variant in BRCA1 or BRCA2
- BRCA1 or BRCA2 pathogenic variant found in a tumor (known as a somatic variant)
Genetic counseling may still be helpful if someone does not meet the above criteria for genetic counseling themselves, but a close relative does. A genetic counselor can determine whether genetic testing is appropriate and who in the family should be tested first.
Genetic counselors can also help with gaining insurance preauthorization for genetic testing. Insurance coverage for testing varies, but testing is covered for many people with the risk factors listed above.
BRCA status may affect cancer treatment decisions. For example, people with BRCA1 or BRCA2 mutations and certain types of breast, ovarian, prostate, and pancreatic cancers may be offered a type of medication called a PARP inhibitor. They should discuss these treatment options with their oncology team.
In addition to the risk factors listed above, the medical care team should consider other factors when determining a person’s risk, such as family size, number of female relatives, preventive breast and gynecological surgeries, and adoption. A full risk assessment should also consider risk factors for other forms of hereditary cancer.
NCCN Genetic Breast, Ovarian, & Pancreatic 3.2024, Benafif 2015, De Felice 2017, Domchek 2016
This article was updated March 22, 2024.

My Gene Counsel ©